Mental health practices across the United States are experiencing a rapid increase in patient demand. As behavioral health awareness grows, providers such as therapists, psychologists, psychiatrists, and counseling centers are seeing higher patient volumes and more complex reimbursement requirements. While patient care remains the top priority, managing the financial side of a mental health practice has become increasingly challenging.
Mental health medical billing plays a critical role in ensuring providers receive accurate and timely reimbursement for the services they deliver. Unlike general healthcare billing, billing for mental health involves unique coding standards, therapy session documentation, insurance verification, and compliance with payer-specific guidelines.
When billing is not handled properly, practices can face delayed payments, claim denials, and revenue loss. This is why many clinics are turning toward professional mental health billing services to streamline their operations and focus more on patient care.
This guide explains how mental health billing works, common challenges providers face, and why specialized billing support is becoming essential for modern behavioral health practices.
Why Mental Health Medical Billing Is Different from General Medical Billing
Mental health billing has several unique aspects that make it more complex than standard healthcare billing.
First, therapy sessions are typically time-based. Insurance payers require specific CPT codes depending on the duration and type of therapy session. Incorrect coding can easily lead to claim denials.
Second, documentation requirements are strict. Therapists and mental health professionals must record detailed notes that justify the services provided. These records must align with the CPT codes submitted in claims.
Third, insurance coverage for mental health services varies widely between payers. Some plans limit the number of sessions, while others require pre-authorizations.
Because of these complexities, many providers rely on mental health billing specialist companies that understand the nuances of coding and billing for mental health services.
Key Components of Mental Health Billing
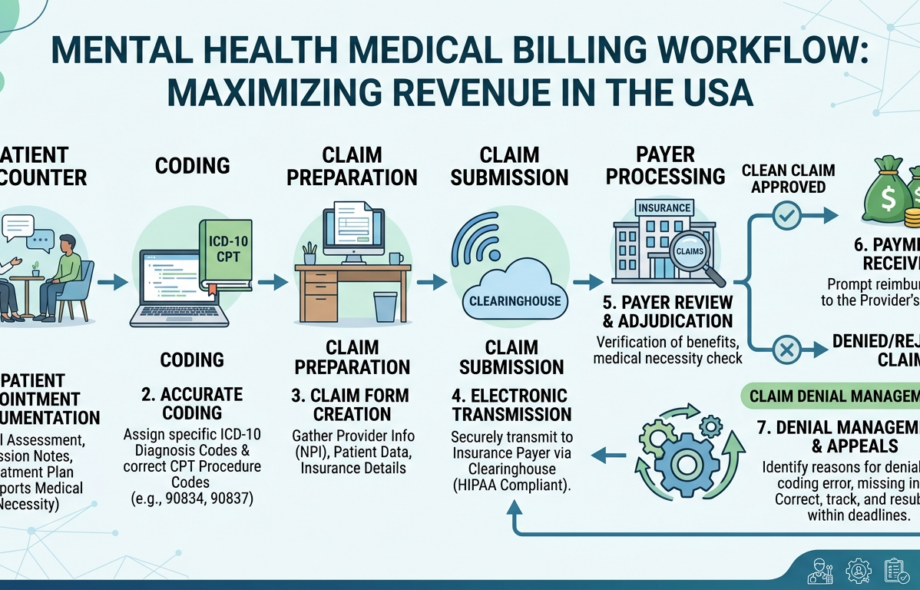
A successful mental health billing process involves multiple steps that must work together seamlessly.
Insurance Verification
Before treatment begins, insurance benefits must be verified. This includes confirming coverage, copays, deductibles, and session limits. Accurate verification helps avoid unexpected billing issues later.
Accurate CPT and ICD Coding
Proper coding is essential for billing mental health services. CPT codes represent the therapy services provided, while ICD diagnosis codes support the medical necessity of treatment.
Professional teams specializing in coding and billing for mental health services ensure claims are submitted correctly the first time.
Claim Submission
Once coding is completed, claims are submitted to insurance companies electronically. Timely submission increases the chances of faster reimbursement.
Practices working with billing companies for mental health often see improved claim acceptance rates due to accurate submissions.
Payment Posting and Reconciliation
After claims are processed, payments from insurers and patients must be posted accurately. This step ensures financial records remain correct and transparent.
Denial Management
Denied claims must be analyzed, corrected, and resubmitted quickly. Efficient denial management is essential for protecting practice revenue.
Common Challenges in Billing for Mental Health Providers
Mental health providers frequently face several challenges when managing billing internally.
One major challenge is frequent claim denials. Insurance companies often reject claims due to incorrect coding, missing documentation, or lack of authorization.
Another challenge is constantly changing insurance regulations. Policies related to billing medicare for mental health services or private insurance reimbursement are regularly updated.
Staff training can also become a burden for clinics trying to keep up with evolving billing rules.
Because of these factors, many practices consider outsourcing mental health billing and coding to experienced professionals who stay updated with payer requirements.
Benefits of Outsourcing Mental Health Billing
Outsourcing has become a common strategy for behavioral health practices that want to reduce administrative stress while improving revenue performance.
Improved Accuracy
Specialized mental health billing services focus entirely on behavioral health billing, which improves coding accuracy and reduces claim rejections.
Faster Reimbursements
Experienced billing teams know how to submit clean claims, resulting in quicker insurance processing and faster payments.
Reduced Administrative Work
When providers choose outsourcing mental health billing, they can shift time and resources back to patient care instead of administrative tasks.
Better Compliance
Regulatory compliance is critical in healthcare billing. Professional behavioral and mental health billing services help ensure claims meet payer and government regulations.
How to Choose the Right Mental Health Billing Company
Selecting the right billing partner is an important decision for any behavioral health practice.
A reliable mental health billing company should have strong experience working with therapy clinics, counseling centers, and psychiatric practices.
Providers should also look for transparency in reporting, consistent communication, and proven expertise in billing for mental health therapists.
The best mental health billing company will provide customized solutions tailored to the needs of individual practices.
Many clinics also evaluate technology capabilities, reporting tools, and claim tracking systems before partnering with a mental health billing services company.
Essential Services Provided by Mental Health Billing Specialists
Professional mental health billing solutions typically include a full range of services designed to support behavioral health practices.
These services often include insurance eligibility verification, prior authorization management, claim submission, denial management, payment posting, and accounts receivable follow-up.
In addition, some mental health billing and credentialing services help providers enroll with insurance networks and maintain credentialing compliance.
Many mental health billing specialist companies also provide financial analytics that help clinics monitor performance and improve revenue cycle efficiency.
Why Behavioral Health Practices Prefer Specialized Billing Services
General medical billing companies may not always understand the complexities of behavioral health claims. This is why many practices prefer working with billing services for mental health clinics that focus specifically on behavioral healthcare.
Specialized billing teams understand therapy session coding, psychotherapy documentation standards, and insurance policies related to behavioral care.
Because of this expertise, behavioral & mental health billing services can significantly reduce errors and increase reimbursement rates.
Many providers searching for the best mental health billing services often prioritize companies with proven experience in behavioral healthcare billing.
The Growing Demand for Mental Health Billing Solutions
The demand for behavioral healthcare services in the United States has grown significantly over the past decade. With more patients seeking therapy and psychiatric support, clinics are expanding their services and patient capacity.
However, growth also brings administrative challenges. Larger patient volumes mean more claims, more insurance interactions, and more financial management responsibilities.
This is one reason why outsourced billing for mental health has become increasingly popular among clinics looking for scalable billing support.
From small therapy practices to large behavioral health organizations, many providers now partner with top mental health billing company providers to manage their revenue cycle efficiently.
Choosing Affordable and Reliable Billing Support
While quality and expertise are essential, cost is also an important factor when selecting billing services.
Some practices search for a cheap outsource mental health billing company that still offers professional service and accurate billing support.
However, providers should avoid choosing services based solely on price. The best outsource mental health billing and coding services focus on both affordability and high-quality claim management.
Working with experienced billing companies helps reduce claim denials, improve reimbursement rates, and strengthen the financial health of the practice.
How Professional Billing Services Improve Practice Growth
Efficient billing processes contribute directly to practice stability and growth.
When billing operations run smoothly, providers experience consistent revenue flow, fewer financial disruptions, and better operational efficiency.
This allows therapists and clinicians to dedicate more time to delivering care rather than dealing with administrative work.
Reliable billing services for mental health providers also help clinics maintain compliance with changing payer rules and documentation standards.
For growing practices, outsourcing billing becomes an effective strategy for managing increased patient volumes without hiring large in-house billing teams.
Organizations like 247 Medical Billing Services support healthcare providers with comprehensive solutions that include medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services. These services help healthcare organizations maintain financial stability while focusing on patient care.
Conclusion
Mental health medical billing is an essential component of every successful behavioral health practice. From accurate coding and claim submission to denial management and payment tracking, every step in the billing process affects a clinic’s financial health.
As billing regulations and insurance policies continue to evolve, managing these responsibilities internally can become overwhelming for many providers.
By partnering with experienced mental health billing services professionals, clinics can improve billing accuracy, reduce claim denials, and maintain a steady revenue stream. With the right billing strategy and support, mental health providers can focus on their primary mission of delivering quality care while maintaining a financially stable practice.
Frequently Asked Questions
What is mental health medical billing?
Mental health medical billing refers to the process of submitting and managing insurance claims for therapy, counseling, psychiatric, and other behavioral health services provided to patients.
Why is mental health billing different from general medical billing?
Mental health billing involves time-based therapy codes, specialized documentation requirements, and payer-specific coverage rules, making it more complex than general healthcare billing.
Should mental health providers outsource their billing?
Many providers choose outsourcing mental health billing because it reduces administrative workload, improves claim accuracy, and helps ensure faster reimbursements.
What services are included in mental health billing services?
Mental health billing services usually include insurance verification, coding, claim submission, denial management, payment posting, and accounts receivable follow-up.
How can a mental health billing company help increase revenue?
A professional mental health billing company improves coding accuracy, reduces claim denials, speeds up reimbursement cycles, and ensures compliance with insurance regulations, ultimately helping practices maintain stable revenue.
 :
https://www.247medicalbillingservices.com/
:
https://www.247medicalbillingservices.com/